Understanding Decubitus Ulcers and Why Immediate Treatment Matters
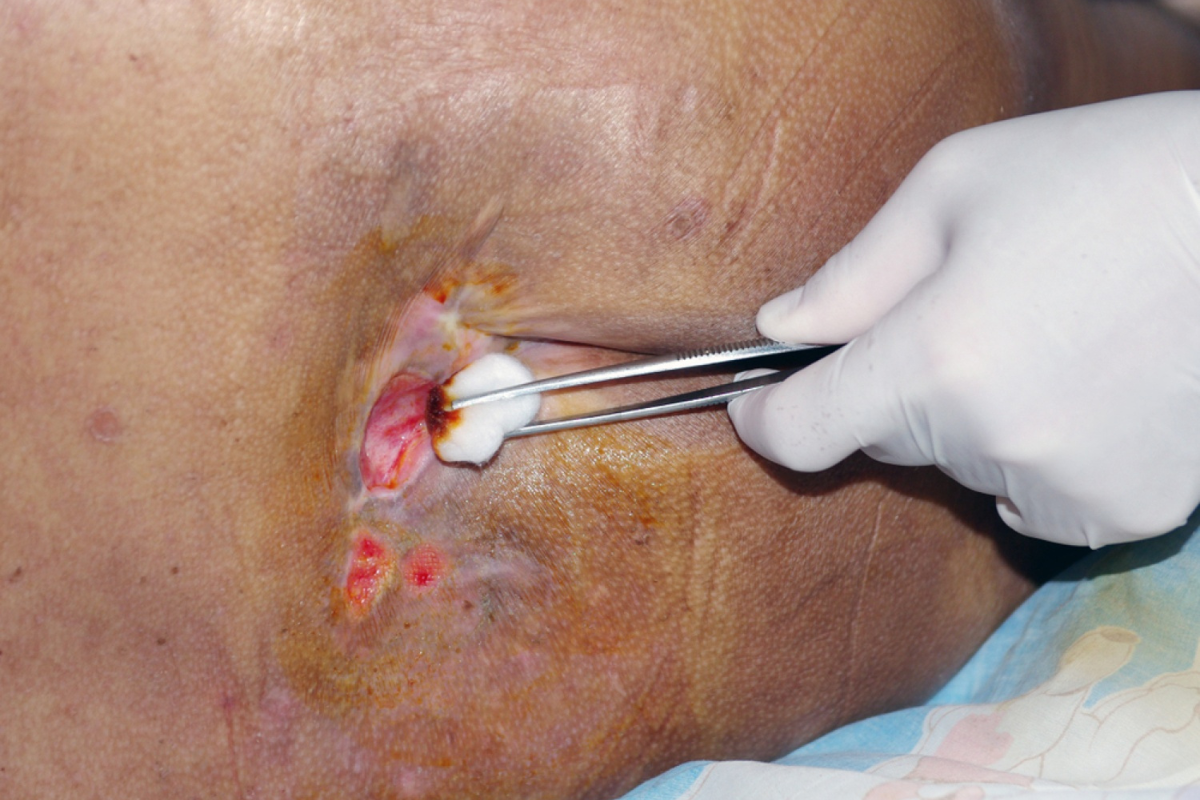
Decubitus ulcer treatment begins with a clear understanding of what these wounds are and how they develop. Also known as pressure ulcers or bedsores, these injuries occur when prolonged pressure cuts off blood flow to the skin and underlying tissues. Over time, the lack of circulation leads to tissue damage, which can worsen rapidly without proper care. These ulcers commonly form in areas where bones are close to the skin, such as the hips, heels, tailbone, and elbows. Individuals who are bedridden or have limited mobility face the highest risk, making prevention and early intervention essential. Ignoring early signs can lead to deeper wounds, infections, and serious complications. Acting quickly with proper decubitus ulcer treatment significantly improves healing outcomes and reduces long-term health risks.
Causes and Risk Factors That Lead to Pressure Ulcers
Several factors contribute to the development of pressure ulcers, and recognizing them is key to effective decubitus ulcer treatment. Continuous pressure is the primary cause, especially when a person remains in one position for extended periods. Friction and shear forces also damage the skin, particularly when patients slide down in beds or chairs. Moisture from sweat, urine, or wound drainage weakens the skin barrier and increases vulnerability. Poor nutrition plays a significant role, as the body needs adequate nutrients to maintain and repair skin tissue. Chronic conditions such as diabetes and vascular disease further impair healing and circulation. Aging skin is thinner and less elastic, making elderly individuals more susceptible to breakdown. Addressing these risk factors is a foundational step in both prevention and treatment strategies.
Stages of Pressure Ulcers and Corresponding Treatment Approaches
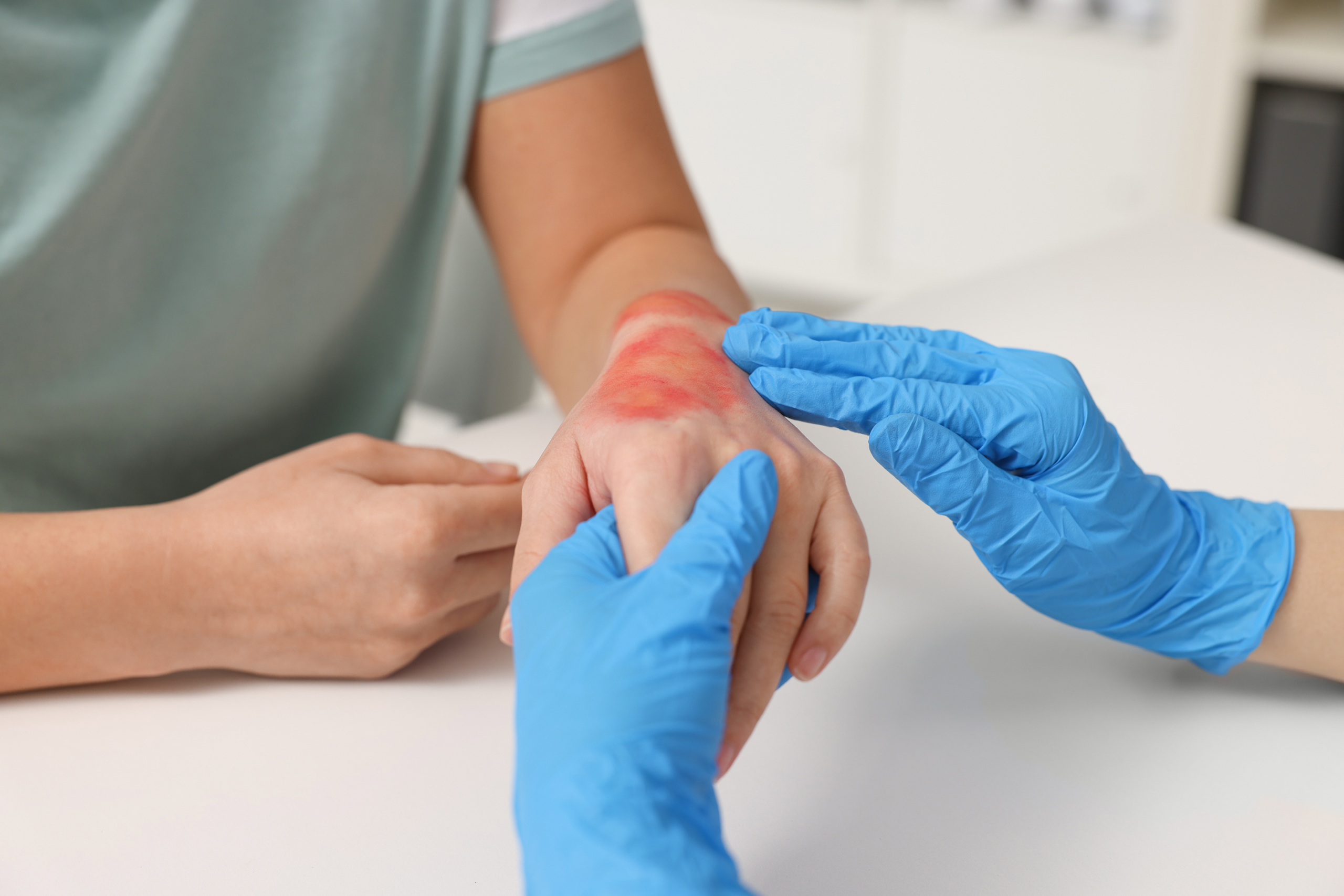
Decubitus ulcer treatment varies depending on the stage of the wound, and understanding these stages helps guide proper care. In Stage 1, the skin appears red and may feel warm or tender, but it remains intact, making early intervention highly effective. Stage 2 involves partial skin loss, often presenting as blisters or shallow open sores that require gentle wound care and protective dressings. Stage 3 ulcers extend deeper into the tissue, exposing fat and requiring more advanced wound management techniques. Stage 4 represents severe damage, with exposure of muscle or bone, often necessitating surgical intervention. Some ulcers are classified as unstageable when debris covers the wound, making it difficult to assess depth. Deep tissue injuries may also develop beneath intact skin, requiring close monitoring. Tailoring decubitus ulcer treatment to each stage ensures the most appropriate and effective care plan.
Core Principles of Decubitus Ulcer Treatment
Successful decubitus ulcer treatment relies on a combination of essential care principles that support healing and prevent further damage. Relieving pressure is the most critical step, often achieved by repositioning the patient every two hours. Support surfaces such as specialized mattresses and cushions help distribute weight more evenly. Keeping the skin clean and dry reduces the risk of infection and further irritation. Improving circulation through gentle movement and positioning enhances the delivery of oxygen and nutrients to the affected area. Managing underlying health conditions ensures that the body can focus on healing. Consistency in these practices is vital, as even minor lapses can delay recovery. A structured care routine makes a significant difference in outcomes.
Wound Care Techniques for Faster Healing
Proper wound care is a cornerstone of effective decubitus ulcer treatment and requires attention to detail. Cleaning the wound with appropriate solutions helps remove debris and bacteria without causing further irritation. Debridement is often necessary to eliminate dead tissue, allowing healthy tissue to grow. Different methods of debridement include autolytic, enzymatic, mechanical, and surgical approaches, depending on the severity of the wound. Choosing the right dressing is equally important, as it maintains moisture balance and protects the area from contamination. Infection control is a constant priority, with antibiotics used when necessary to manage bacterial growth. Monitoring the wound regularly helps track progress and identify any complications early. Consistent and careful wound care significantly accelerates healing.
Advanced Medical Treatments and Technologies
Modern medicine offers several advanced options for decubitus ulcer treatment, particularly for severe or non-healing wounds. Negative pressure wound therapy uses controlled suction to remove excess fluid and promote tissue growth. Skin grafting may be required for deep ulcers that cannot heal on their own. Biologic dressings and growth factors support the regeneration of healthy tissue. Hyperbaric oxygen therapy enhances oxygen delivery to damaged areas, improving healing potential. Electrical stimulation has also shown promise in encouraging tissue repair. These advanced treatments are typically recommended by specialists based on individual patient needs. Access to these options can greatly improve outcomes for complex cases.
The Role of Nutrition in Decubitus Ulcer Treatment
Nutrition plays a vital role in the effectiveness of decubitus ulcer treatment, as the body requires adequate resources to repair damaged tissue. Protein is essential for rebuilding skin and supporting immune function. Vitamins such as Vitamin C contribute to collagen production and wound healing. Zinc aids in tissue repair and helps strengthen the immune response. Proper hydration maintains skin elasticity and supports overall bodily functions. Malnutrition can significantly delay healing and increase the risk of complications. A well-balanced diet tailored to the patient’s needs enhances recovery speed. Nutritional support should always be part of a comprehensive care plan.
Preventing Infection and Managing Complications
Infection prevention is a critical component of decubitus ulcer treatment, as open wounds are highly vulnerable to bacteria. Early signs of infection include redness, swelling, foul odor, and unusual discharge. Maintaining proper hygiene reduces the risk of contamination and supports healing. Pain management is also important, as discomfort can affect mobility and overall well-being. Severe complications such as sepsis can arise if infections are left untreated. Regular monitoring allows caregivers to respond quickly to any changes in the wound. Timely medical intervention ensures that complications are addressed before they escalate. Vigilance is key to successful treatment.
Home Care Strategies for Managing Pressure Ulcers
Caring for pressure ulcers at home requires dedication, consistency, and proper knowledge of decubitus ulcer treatment techniques. Daily skin inspections help identify early signs of breakdown before they worsen. Repositioning the patient frequently prevents prolonged pressure on vulnerable areas. Using supportive devices such as cushions and mattresses improves comfort and reduces risk. Caregivers play a crucial role in maintaining hygiene and ensuring that wound care routines are followed. Creating a clean and safe environment supports healing and minimizes infection risks. Education and training empower caregivers to provide effective support. Home care can be highly effective when done correctly and consistently.
Key Home Care Practices for Better Healing
- Reposition the patient every two hours to relieve pressure
- Keep the skin clean and dry at all times
- Use pressure-relieving mattresses and cushions
- Inspect the skin daily for any changes or signs of damage
- Ensure proper nutrition and hydration
- Follow prescribed wound care routines carefully
- Seek medical advice if the wound shows signs of worsening
Professional Medical Care and When It Is Necessary
While home care is essential, there are times when professional medical care becomes necessary for effective decubitus ulcer treatment. Healthcare providers can assess the severity of the ulcer and recommend appropriate interventions. Wound care specialists have access to advanced treatments that may not be available at home. Hospital-based care may be required for severe infections or complications. Long-term care planning is often needed for patients with chronic conditions. Regular follow-ups ensure that treatment plans remain effective and are adjusted as needed. Professional guidance enhances the chances of successful healing.
Lifestyle Adjustments to Support Long-Term Healing
Long-term healing from pressure ulcers requires meaningful lifestyle adjustments alongside decubitus ulcer treatment. Improving mobility, even through small movements, helps reduce pressure and improve circulation. Establishing a consistent skin care routine protects against future breakdown. Managing chronic illnesses such as diabetes ensures better overall health and healing capacity. Staying hydrated and maintaining a balanced diet supports ongoing recovery. Regular medical check-ups help monitor progress and prevent recurrence. These adjustments contribute to both healing and prevention. A proactive approach makes a lasting difference.
Takeaway
Decubitus ulcer treatment demands a comprehensive approach that combines proper wound care, pressure relief, nutrition, and medical support. Early detection and consistent care are the most powerful tools in preventing complications and promoting recovery. Whether managed at home or in a clinical setting, attention to detail and commitment to routine play a vital role. Caregivers and patients alike benefit from understanding the causes, stages, and treatment options available. With the right strategies in place, healing becomes more achievable and sustainable.
Frequently Asked Questions (FAQ)
What is the fastest way to start decubitus ulcer treatment
The fastest way is to relieve pressure on the affected area, clean the wound properly, and apply appropriate dressings while seeking medical advice.
Can decubitus ulcers heal without medical treatment
Mild ulcers may improve with proper care, but medical supervision is strongly recommended to ensure safe and complete healing.
How long does decubitus ulcer treatment take
Healing time varies depending on the severity of the ulcer and the patient’s overall health, ranging from weeks to several months.
Are decubitus ulcers preventable
Yes, regular repositioning, proper nutrition, and consistent skin care can significantly reduce the risk of developing pressure ulcers.
What are the warning signs that a pressure ulcer is getting worse
Signs include increased pain, swelling, foul odor, pus, and fever, all of which require immediate medical attention.
What type of mattress is best for pressure ulcer treatment
Pressure-relieving mattresses such as foam or alternating pressure systems are commonly recommended for reducing pressure points.
Is surgery always required for severe pressure ulcers
Surgery is only necessary in advanced cases where other treatments are not effective or when there is extensive tissue damage.