Understanding Wound Care Assessment
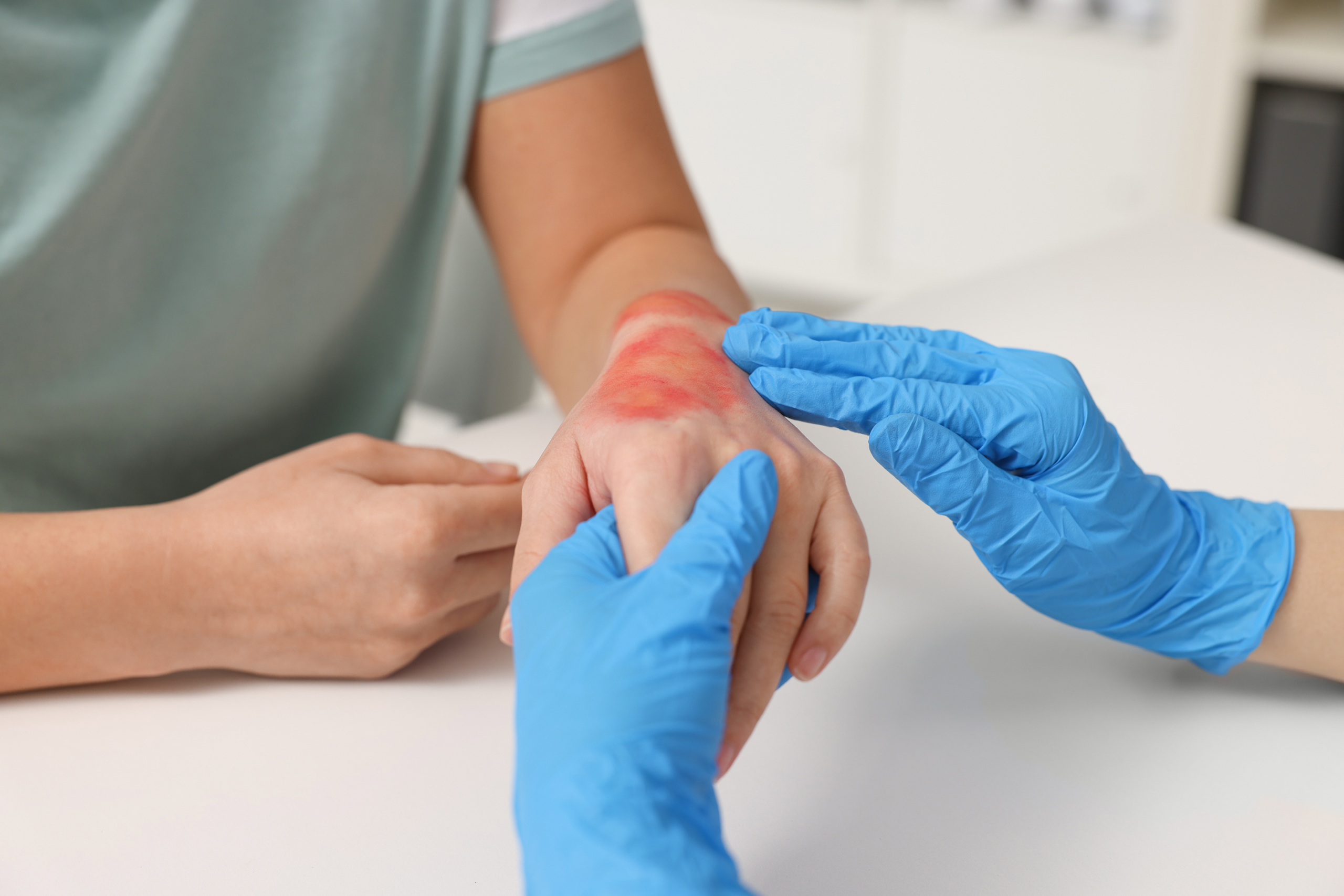
Wound care assessment is a structured clinical process used to evaluate the condition of a wound and guide appropriate treatment decisions. It involves careful observation, measurement, and documentation of wound characteristics to understand healing progress. Healthcare professionals rely on wound care assessment to identify complications early and adjust care plans effectively. This process is essential in both acute and chronic wound management because it ensures that every stage of healing is properly monitored. A consistent approach to wound care assessment improves communication between care teams and supports better patient outcomes. It also helps determine whether a wound is healing as expected or requires additional intervention. Accurate assessment forms the foundation of effective wound management across all healthcare settings.
Importance of Wound Care Assessment in Clinical Practice
Wound care assessment plays a vital role in modern healthcare because it directly influences treatment success and patient recovery. Without proper evaluation, wounds may worsen, leading to infection or delayed healing. Clinicians use wound care assessment to make informed decisions that prevent complications and improve quality of life for patients. It also supports early identification of risk factors that may interfere with healing. In many cases, structured assessment reduces unnecessary treatments and optimizes resource use. It is also essential for maintaining continuity of care when multiple healthcare providers are involved. Proper wound evaluation ensures that treatment adjustments are based on real and measurable changes rather than assumptions.
Key reasons why wound care assessment is essential include:
- Early detection of infection or tissue deterioration
- Improved accuracy in treatment planning
- Better tracking of healing progress over time
- Enhanced coordination among healthcare professionals
- Reduction in long-term healthcare costs
- Support for evidence-based clinical decisions
Each of these elements contributes to safer and more effective patient care. Consistent assessment ensures that no critical detail is overlooked during treatment.
Key Objectives of Wound Care Assessment
The main goal of wound care assessment is to gather detailed and accurate information about a wound’s condition. This information helps healthcare providers determine the most effective treatment strategy. Another important objective is to identify the underlying cause of the wound, especially in chronic cases. Monitoring changes over time is also essential to determine whether healing is progressing normally. Wound care assessment also helps evaluate the effectiveness of current interventions and guides necessary adjustments. It ensures that care remains patient-centered and responsive to changing conditions. A structured assessment process allows clinicians to maintain a clear picture of wound status at all times.
Additional objectives include:
- Identifying wound type and severity
- Monitoring healing progression
- Detecting complications early
- Guiding dressing and treatment selection
- Evaluating surrounding skin condition
- Supporting long-term wound management strategies
These objectives ensure that care remains structured and consistent throughout the healing process.
Types of Wounds Requiring Assessment
Wounds vary widely in cause, severity, and healing potential, making wound care assessment essential for all types. Acute wounds typically result from trauma or surgery and usually heal within a predictable timeframe. Chronic wounds, however, may persist for weeks or months and require ongoing evaluation. Pressure injuries, diabetic ulcers, and venous leg ulcers are among the most common chronic wound types. Each category requires a tailored approach to assessment and treatment. Understanding wound classification helps clinicians choose appropriate interventions. Proper identification of wound type also reduces the risk of incorrect management strategies.
Common wound types include:
- Acute wounds such as cuts and surgical incisions
- Chronic wounds that fail to heal within expected timeframes
- Pressure injuries caused by prolonged pressure on skin
- Diabetic foot ulcers related to poor circulation and nerve damage
- Venous and arterial ulcers affecting lower limbs
- Traumatic wounds from accidents or injuries
- Burns caused by heat, chemicals, or electricity
Each wound type presents unique challenges that must be carefully evaluated during wound care assessment.
Step-by-Step Wound Care Assessment Process
Wound care assessment follows a structured process that ensures no important detail is missed. The first step involves reviewing the patient’s medical history and identifying any underlying conditions that may affect healing. Next, a physical examination is performed to evaluate the wound and surrounding tissue. Measurement of the wound’s dimensions is then completed using standardized tools. The wound bed is carefully examined to identify tissue types such as granulation or necrotic tissue. Periwound skin is also assessed for signs of damage or irritation. Each step builds a clearer clinical picture of wound status.
Key steps include:
- Reviewing patient history and risk factors
- Performing a full physical examination
- Measuring wound length, width, and depth
- Evaluating wound bed characteristics
- Assessing surrounding skin condition
- Analyzing wound drainage and exudate
- Identifying pain levels and infection signs
Each step contributes to a complete understanding of the wound’s condition and supports accurate clinical decision-making.
Tools and Technologies Used in Wound Care Assessment
Modern wound care assessment relies on both traditional tools and advanced technologies. Basic tools such as rulers and probes are still widely used for measurement. However, digital imaging systems have significantly improved accuracy and documentation. Mobile applications now allow clinicians to track wound progress over time with greater precision. Standardized assessment tools help ensure consistency across different healthcare providers. Electronic health records also play a major role in storing and sharing wound data. These innovations have transformed how wound progress is monitored in clinical practice.
Common tools and technologies include:
- Measuring rulers and depth probes
- Digital wound photography systems
- Mobile wound tracking applications
- PUSH and Bates-Jensen assessment tools
- Electronic health record systems
- Tissue oxygenation monitoring devices
These tools improve accuracy, efficiency, and communication in wound management. They also support long-term tracking of healing outcomes.
Factors That Affect Wound Healing
Wound healing is influenced by multiple internal and external factors that must be considered during wound care assessment. Patient health status plays a significant role, especially in individuals with chronic conditions such as diabetes. Nutrition and hydration levels also affect tissue repair and regeneration. Circulatory health determines how well oxygen and nutrients reach the wound site. Lifestyle choices such as smoking can significantly delay healing. Age is another important factor, as older individuals may experience slower recovery. Environmental and behavioral factors also contribute to healing outcomes.
Key influencing factors include:
- Chronic diseases such as diabetes and vascular disorders
- Poor nutrition and dehydration
- Reduced blood circulation
- Smoking and alcohol consumption
- Medication effects on healing
- Limited mobility or physical inactivity
- Age-related physiological changes
Understanding these factors allows healthcare providers to adjust treatment plans accordingly and improve healing potential.
Documentation Best Practices in Wound Care Assessment
Accurate documentation is essential in wound care assessment because it ensures continuity and accountability. Clear and consistent records help healthcare teams track progress effectively. Proper documentation also supports clinical decision-making and legal compliance. Wound descriptions must be detailed, objective, and updated regularly. Photographic documentation is often used to complement written records. Standardized terminology helps avoid confusion among care providers. Good documentation strengthens communication between healthcare professionals.
Best practices include:
- Using consistent measurement techniques
- Recording wound characteristics clearly and objectively
- Updating records after each assessment
- Including photographic evidence when appropriate
- Using standardized wound care terminology
- Ensuring data accuracy across all entries
High-quality documentation improves patient safety and supports long-term care planning.
Common Mistakes in Wound Care Assessment and How to Avoid Them
Errors in wound care assessment can lead to delayed healing or improper treatment. One common mistake is inconsistent measurement techniques, which can distort healing progress. Another issue is incomplete documentation that omits important clinical details. Some clinicians may overlook changes in surrounding skin, which can indicate complications. Misidentifying wound types can also result in ineffective treatment plans. Regular reassessment is sometimes neglected, leading to outdated care decisions. These mistakes can significantly affect patient outcomes if not addressed properly.
Common mistakes include:
- Inconsistent wound measurement methods
- Incomplete or unclear documentation
- Failure to monitor periwound skin
- Incorrect wound classification
- Lack of regular reassessment
- Ignoring patient-reported symptoms
Avoiding these errors ensures more accurate wound care assessment and improved healing outcomes.
Role of Healthcare Professionals in Wound Care Assessment
Wound care assessment involves collaboration among various healthcare professionals. Nurses often perform routine evaluations and monitor changes in wound condition. Physicians are responsible for diagnosing underlying causes and prescribing treatment. Wound care specialists provide advanced expertise for complex cases. Home healthcare providers ensure continuity of care outside clinical settings. Each professional contributes to a comprehensive care plan that supports healing. Collaboration improves accuracy and consistency in wound evaluation.
Their responsibilities include:
- Monitoring wound progression regularly
- Identifying complications early
- Adjusting treatment plans as needed
- Educating patients on wound care practices
- Coordinating care across different settings
Teamwork ensures that wound care assessment remains accurate, consistent, and patient-focused.
Wound Care Assessment in Different Settings
Wound care assessment is performed in various healthcare environments depending on patient needs. Hospitals handle acute and severe wound cases requiring immediate attention. Long-term care facilities manage chronic wounds that need ongoing monitoring. Home healthcare settings provide personalized care for patients with mobility limitations. Outpatient clinics focus on follow-up assessments and treatment adjustments. Emergency departments assess traumatic wounds requiring urgent care. Each setting requires tailored approaches while maintaining core assessment principles.
Consistency across settings ensures accurate tracking of wound progress. Communication between healthcare environments supports continuity of care. This reduces the risk of mismanagement or incomplete treatment plans.
Patient Education and Engagement in Wound Care Assessment Process
Patient involvement is an important part of wound care assessment because it improves adherence to treatment plans. Educating patients helps them understand how to monitor their wounds at home. It also encourages them to recognize early signs of complications. Patients who are actively engaged tend to experience better healing outcomes. Healthcare providers play a key role in simplifying complex medical information for patients. Clear communication improves cooperation and confidence in care plans.
Patient education often includes:
- Proper wound cleaning techniques
- Dressing change instructions
- Warning signs of infection
- Importance of nutrition and hydration
- Lifestyle changes that support healing
Active participation strengthens the effectiveness of wound care assessment and overall treatment success.
Advanced Approaches in Wound Care Assessment
Advancements in medical technology have significantly improved wound care assessment methods. Digital imaging allows for more precise tracking of wound changes over time. Biofilm detection techniques help identify hidden infections that delay healing. Tissue oxygen measurement provides insight into circulation and healing potential. Predictive analytics is increasingly used to forecast healing outcomes based on patient data. These innovations enhance the accuracy and efficiency of clinical evaluations. They also support more personalized treatment strategies.
Advanced approaches include:
- Digital wound imaging systems
- Biofilm detection technologies
- Oxygenation and perfusion measurement tools
- Predictive data modeling for healing outcomes
- Moisture balance analysis systems
These methods improve clinical decision-making and patient care quality.
When to Escalate Care Based on Wound Care Assessment Findings
Certain signs during wound care assessment indicate the need for urgent medical intervention. Rapid deterioration of the wound is a key warning sign. Increased redness, swelling, or discharge may suggest infection. Severe pain that worsens over time also requires attention. Systemic symptoms such as fever indicate possible spreading infection. Lack of healing progress over an extended period is another concern. Early escalation helps prevent serious complications.
Escalation may be necessary when:
- Wound size increases unexpectedly
- Signs of infection become more severe
- Pain becomes unmanageable
- Systemic symptoms develop
- No improvement is observed over time
Timely action ensures better patient outcomes and prevents further complications.
Frequently Asked Questions
What is wound care assessment used for?
It is used to evaluate wound condition, guide treatment decisions, and monitor healing progress over time.
How often should wound care assessment be done?
Frequency depends on wound type, but chronic wounds often require regular reassessment, sometimes weekly or more frequently.
What are the key components of wound care assessment?
Key components include wound measurement, tissue evaluation, drainage analysis, pain assessment, and infection monitoring.
Why is documentation important in wound care assessment?
It ensures continuity of care, supports clinical decisions, and provides accurate records for monitoring progress.
Can wound care assessment be done at home?
Basic monitoring can be done at home, but professional assessment is necessary for accurate evaluation and treatment adjustments.
Takeaway
Wound care assessment is a structured and essential clinical process that ensures wounds are properly evaluated, monitored, and managed throughout healing. It supports accurate diagnosis, timely intervention, and effective treatment planning across all healthcare settings. Consistent assessment improves communication among healthcare professionals and enhances patient outcomes. When combined with proper documentation, advanced tools, and patient involvement, wound care assessment becomes a powerful foundation for successful wound management.