Overview of Severe Wound Surgery Topic
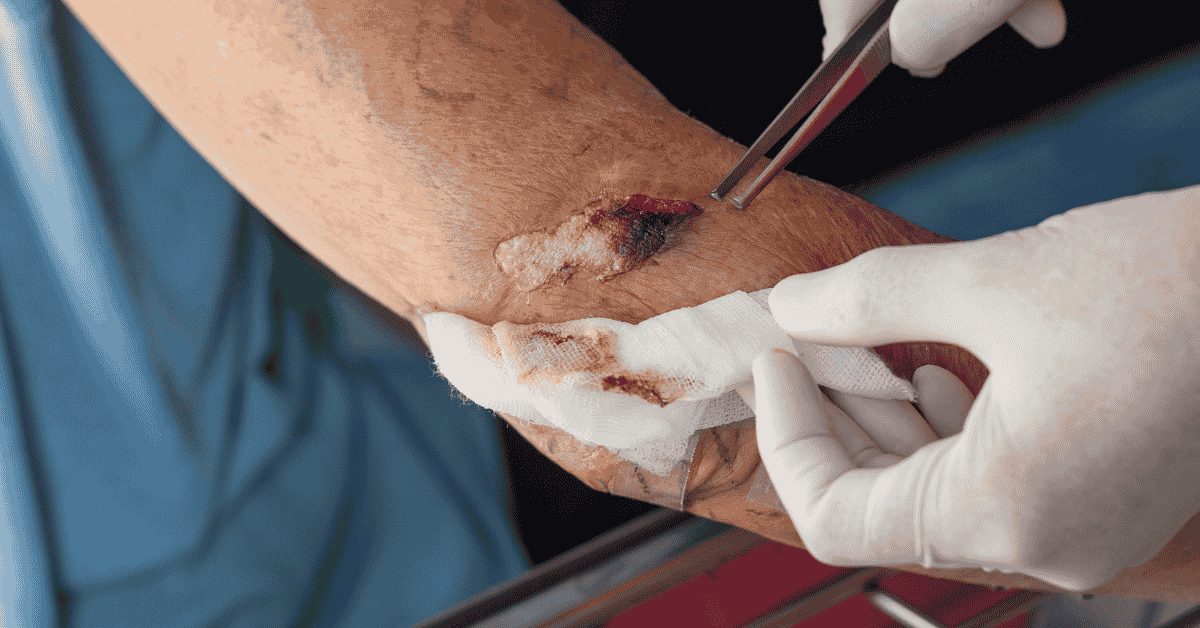
Sever wound surgery refers to specialized surgical procedures used to treat deep, complex, and often life-threatening injuries involving skin, muscle, nerves, blood vessels, or bone. These types of injuries usually occur when tissue damage exceeds the body’s natural ability to heal without medical intervention. In many cases, sever wound surgery becomes necessary in emergency settings where immediate care can prevent long-term disability or infection. Medical teams prioritize restoring function, controlling bleeding, and preventing contamination during treatment. The scope of this surgical field includes emergency trauma care, reconstructive techniques, and long-term restoration of affected areas. Patients undergoing sever wound surgery often require multidisciplinary care involving surgeons, nurses, and rehabilitation specialists. The overall goal is not only survival but also restoring as much physical function and appearance as possible.
Understanding Severe Wounds
Severe wounds come in multiple forms, each with different levels of complexity and tissue involvement. Deep lacerations often involve sharp trauma that cuts through multiple layers of skin and muscle. Avulsion injuries occur when tissue is forcibly detached from the body, often requiring reconstructive sever wound surgery. Puncture wounds may seem small externally but can cause deep internal damage and infection risks. Crush injuries typically involve heavy pressure that damages muscles, bones, and blood vessels simultaneously. Burn-related injuries can destroy large areas of skin and underlying structures, requiring surgical reconstruction. Each type of wound is assessed based on depth, contamination level, and structural damage to determine surgical needs.
When Severe Wound Surgery Becomes Necessary
Sever wound surgery becomes necessary when tissue damage is too extensive for natural healing processes. One key indicator is the presence of dead or non-viable tissue that must be surgically removed. Heavy bleeding that cannot be controlled through basic medical care often requires surgical intervention. Infection signs such as pus, swelling, and severe redness may also indicate the need for surgical cleaning. Damage involving nerves, arteries, or muscles typically requires reconstructive procedures. In many cases, non-surgical treatments fail to restore proper function, making sever wound surgery the most effective option. Medical professionals evaluate each case carefully before deciding on surgical treatment.
Emergency Response Prior to Surgery
Before sever wound surgery is performed, emergency response plays a critical role in patient survival. Immediate pressure is applied to control bleeding and reduce blood loss. Cleaning the wound as much as possible helps minimize infection risk before hospital arrival. Immobilizing the injured area prevents further damage during transport. Pain management is often initiated in emergency settings to stabilize the patient. Quick transportation to a surgical facility significantly improves outcomes in severe injury cases. Emergency care sets the foundation for successful surgical treatment.
Diagnostic Evaluation and Medical Imaging
Accurate diagnosis is essential before performing sever wound surgery. A detailed physical examination helps determine visible and internal damage. X-rays are commonly used to assess bone fractures or foreign objects. CT scans provide detailed cross-sectional images of deeper tissue injuries. MRI scans are especially useful for evaluating soft tissue, nerves, and ligaments. Laboratory tests help identify infections or internal bleeding risks. These diagnostic tools allow surgeons to plan precise and effective surgical procedures.
Preoperative Preparation for Severe Wound Surgery
Before sever wound surgery begins, careful preparation ensures patient safety. Stabilizing vital signs such as blood pressure and heart rate is a priority. Anesthesia planning is conducted to ensure the patient remains pain-free during the procedure. Infection control measures are implemented to reduce surgical risks. The affected area is cleaned and sterilized thoroughly before incision. Medical teams assess overall health conditions that may affect surgery outcomes. Proper preparation increases the likelihood of successful healing and recovery.
Surgical Techniques Used in Severe Wound Surgery
Sever wound surgery involves multiple advanced techniques depending on injury severity. Debridement is performed to remove dead or contaminated tissue from the wound. Irrigation techniques are used to flush out bacteria and debris. Skin grafting helps replace damaged skin with healthy tissue from another area. Flap surgery may be required for more complex wounds involving deeper structures. Vascular repair restores proper blood flow to injured regions. Nerve repair techniques aim to recover sensation and movement when possible. These surgical methods are often combined for optimal results.
Role of Antibiotics and Infection Control
In sever wound surgery, infection prevention is a critical concern throughout treatment. Antibiotics are often administered before and after surgery to reduce bacterial growth. Sterile environments are strictly maintained during surgical procedures. Surgeons continuously monitor wounds for early signs of infection. Proper wound dressing techniques help protect the surgical site during healing. Infection control protocols significantly reduce complications after surgery. Without proper infection management, recovery outcomes may be severely affected.
Pain Management Strategies
Pain control is an essential part of sever wound surgery treatment. Before surgery, anesthesia ensures the patient remains unconscious or numb during procedures. During surgery, controlled medication helps maintain stability and comfort. After surgery, pain management continues through prescribed medications. Nerve blocks may be used for targeted pain relief in specific areas. Long-term pain management strategies may be necessary depending on injury severity. Effective pain control improves healing and overall patient recovery experience.
Post-Surgical Care and Wound Monitoring
After sever wound surgery, continuous care is required to ensure proper healing. Regular dressing changes help keep the wound clean and protected. Medical staff monitor for signs of infection or complications. Drains may be placed to remove excess fluids from surgical sites. Follow-up visits allow doctors to evaluate healing progress. Patients are often advised to limit movement in affected areas. Careful monitoring ensures long-term surgical success.
Healing Stages After Severe Wound Surgery
Healing after sever wound surgery occurs in multiple stages. The inflammatory stage involves swelling and immune response activation. The regeneration stage focuses on new tissue formation and repair. During the remodeling stage, tissue strengthens and stabilizes over time. Each stage plays a vital role in full recovery. Nutrition and rest significantly influence healing speed. Proper care during each phase improves long-term outcomes.
Complications and Risks Associated with Severe Wound Surgery
Although sever wound surgery is often life-saving, risks may still occur. Infection remains one of the most common complications. Some patients may experience delayed healing due to medical conditions. Scar formation can vary depending on injury severity. In some cases, graft rejection may occur after reconstruction. Loss of function in affected areas is also a possible outcome. Careful medical monitoring helps reduce these risks.
Rehabilitation and Physical Therapy
Rehabilitation is a key part of recovery after sever wound surgery. Physical therapy helps restore strength and mobility in affected areas. Exercises are designed to improve flexibility and function. Occupational therapy may assist patients in returning to daily activities. Recovery programs are customized based on injury severity. Consistent therapy sessions improve long-term outcomes. Rehabilitation ensures patients regain independence over time.
Scarring and Cosmetic Outcomes
Scarring is a natural part of healing after sever wound surgery. The extent of scarring depends on wound depth and treatment methods. Some surgical techniques aim to minimize visible scars. Silicone treatments and specialized creams may improve skin appearance. In certain cases, additional reconstructive procedures may be performed. Emotional impact of visible scars can also affect patients. Supportive care helps address both physical and psychological aspects.
Advances in Severe Wound Surgery
Modern sever wound surgery continues to evolve with new technologies. Negative pressure wound therapy helps accelerate healing. Bioengineered skin substitutes provide alternatives to traditional grafts. Regenerative medicine explores tissue regrowth possibilities. Stem cell research shows promising potential in wound repair. Advanced surgical tools improve precision and outcomes. These innovations continue to transform patient recovery experiences.
Special Considerations in Severe Wound Surgery
Certain patient groups require special attention during sever wound surgery. Individuals with diabetes may experience slower healing rates. Elderly patients often require additional care due to fragile skin. Immunocompromised individuals face higher infection risks. Pediatric patients require specialized surgical approaches. Each case is evaluated individually to ensure safety. Tailored treatment plans improve recovery success.
Hospital vs Outpatient Care Settings
Sever wound surgery is typically performed in hospital environments due to complexity. Hospitals provide advanced equipment and emergency support. Some minor follow-up care may be managed in outpatient settings. Severe cases require continuous monitoring in inpatient care. Decision depends on injury severity and patient condition. Proper setting selection ensures optimal recovery outcomes. Medical supervision remains essential throughout treatment.
Cost Factors and Insurance Considerations
The cost of sever wound surgery varies widely depending on complexity. Surgical procedures involving reconstruction tend to be more expensive. Hospital stay duration also affects total cost. Diagnostic imaging and medications contribute to expenses. Insurance coverage often helps reduce financial burden. Each case is evaluated individually for billing purposes. Understanding costs helps patients prepare for treatment.
Prevention of Severe Wound Complications
Preventing complications is an important aspect of wound care. Safety measures in workplaces reduce injury risks. Immediate medical attention helps prevent worsening conditions. Proper hygiene reduces infection chances. Education about wound care improves patient outcomes. Early intervention often prevents the need for complex surgery. Prevention strategies play a major role in reducing severe injuries.
Frequently Asked Questions (FAQ)
What qualifies as a severe wound requiring surgery?
A severe wound requiring sever wound surgery typically involves deep tissue damage, uncontrolled bleeding, or infection risk that cannot heal naturally. These wounds often include muscle, nerve, or bone involvement.
How long does recovery take after sever wound surgery?
Recovery time varies depending on injury severity, ranging from several weeks to several months. Complex cases may require long-term rehabilitation.
Is sever wound surgery painful?
During surgery, anesthesia prevents pain. After surgery, discomfort is managed through prescribed medications and pain control techniques.
What are the chances of full recovery?
Recovery depends on injury severity, patient health, and timely treatment. Many patients regain significant function with proper care.
Can scars from sever wound surgery be reduced?
Yes, scar reduction treatments such as topical creams, silicone sheets, and additional surgical procedures can improve appearance.
What are the risks of not treating a severe wound surgically?
Without sever wound surgery, risks include infection, permanent disability, tissue death, and life-threatening complications.
Takeaway in the End
Sever wound surgery plays a vital role in treating complex and life-threatening injuries that cannot heal on their own. It combines emergency care, advanced surgical techniques, and long-term rehabilitation to restore function and improve quality of life. Proper diagnosis, timely intervention, and consistent post-surgical care significantly influence recovery outcomes. Modern advancements continue to improve surgical precision and healing success rates. With the right medical approach, many patients experience meaningful recovery even after serious injuries.